 If no pulse is detected, chest compressions must be initiated immediately! Compressions shouldīe given at a rate of 100-120 per minute and a depth of 2-2.4 inches. Assessment must take less than 10 seconds if the diagnosis is uncertain after 10 seconds, proceed as though the patient is indeed in cardiac arrest.(Ref.7)Ĭ: Circulation is the FIRST priority! Check this by palpating the carotid pulse for no more than 10 seconds. Rapidly confirming or refuting the diagnosis of cardiac arrest. 
Initial Actions and Primary Survey All patients who collapse or are found unresponsive should be presumed to be in cardiac arrest until proven otherwise.Īssessment is the first step when encountering such a patient, with the goal of Lives, and high-quality CPR and early defibrillation can improve survival rates.(Ref.6) (Ref.4) Pediatric survival rates for in-hospital arrest are significantly higher than adult rates, currently at approximately 40%.(Ref.4) There are notable racial andĮconomic disparities in cardiac arrest incidence and outcomes, with patients who are black or from lower socioeconomic status more likely to experience cardiac arrest, and less likely to survive.(Ref.4) Basic life support (BLS) is critical to saving This figure has climbed steadily from less than 17% in 2000. More than 300,000 out-of-hospital adult cardiac arrests occur each year in the United States and approximately 10% survive the arrest.(Ref.1-4) Around 200,000 in-hospital adult cardiac arrests occur every year and approximately 25% survive to hospitalĭischarge.(Ref.3-6). Formulate a differential diagnosis for potentially reversible causes of cardiac arrest.Compare and contrast the treatment algorithms for each of the above rhythms. 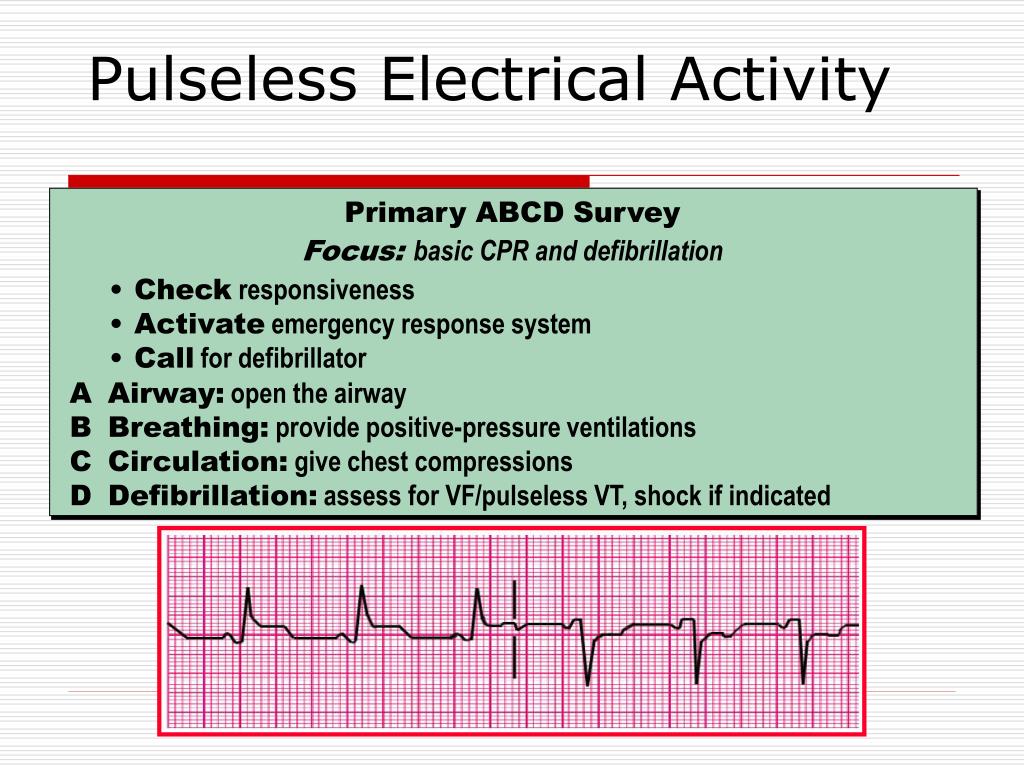 
Identify arrest rhythms on electrocardiogram, including ventricular fibrillation, ventricular tachycardia, pulseless electrical activity, and asystole.Discuss the importance of adequate chest compressions and early defibrillation in the management of pulseless patients.Describe an approach to the initial assessment and stabilization of patients with cardiac arrest.There’s so much happening at once, but what’s the most important thing to do? When it’s your turn to be in charge of a code response, how should you prioritize and make sense of the chaos?īy the end of this module, the student will be able to: A tech is putting defibrillation pads on the patient, one of the residents is trying to ultrasound the patient’s heart, and another is setting up to intubate.Ī nurse comes up with an amp of epinephrine, but the patient doesn’t even have access yet, and your attending is trying to decide whether to activate a STEMI alert. The rest of your team comes rushing in and everyone is talking at once. You realize that he’s apneic and pulseless, so you hit the code buttonĪnd start CPR. 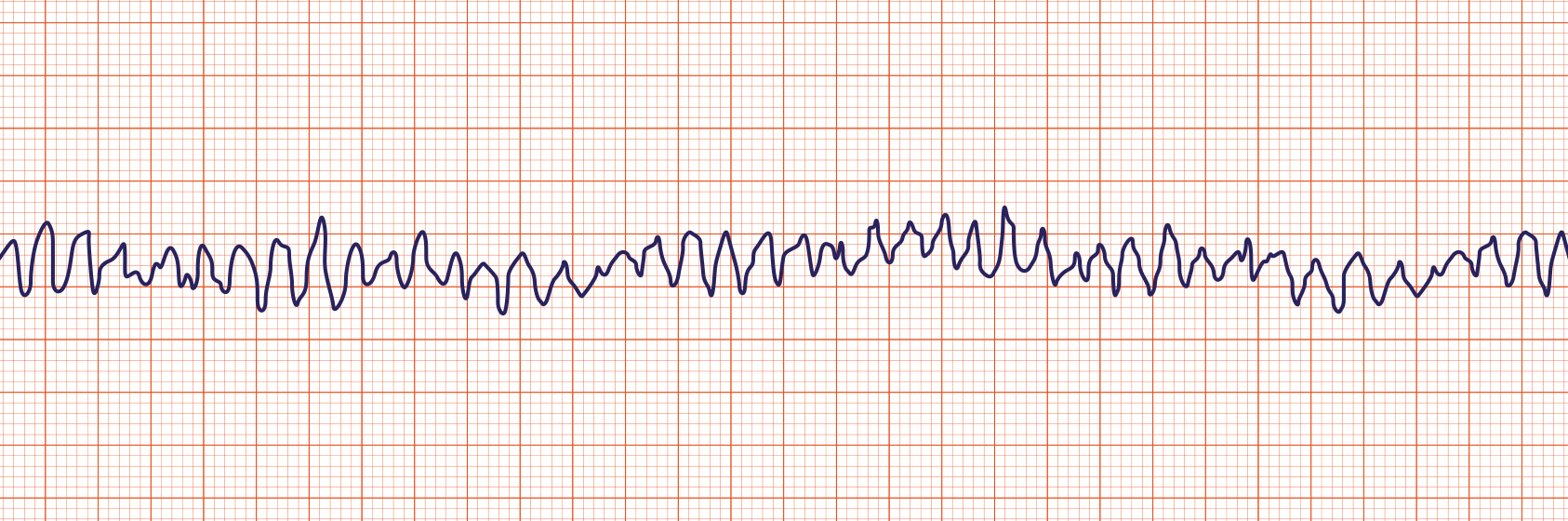
Shortly after arrival, he becomes acutely unresponsive. A 49-year-old man presents to the ED with chest pain. You are a medical student on your Emergency Medicine clerkship. SAEMF/CDEM Innovations in Undergraduate Emergency Medicine Education GrantĬareer Development and Mentorship CommitteeĬDEM Medical Education Fellow Travel Scholarship Virtual Rotation and Educational ResourcesĮMF/SAEMF Medical Student Research Training Grant Visit us on Twitter LinkedIn Facebook YouTube Instagram 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
